Blog

Whose voice in health?
Tuesday September 29, 2020
This year marked the second iteration of the Honourable Roger Cook’s Your Voice in Health engagement survey, which gives WA Health employees the opportunity to share their opinions about their workplace.
Results are dissected in numerous ways, highlighting health service provider (HSP) strengths or areas where improvements are required – all packaged in an official report, which is available on the WA Health website.
Some of the results from the 2019 Your Voice in Health survey were featured in the November 2019 Medicus cover story.
Morale: A close look at clinical engagement & cultures in WA public hospitals. So how do the 2020 Your Voice in Health survey results compare?
Response Rate
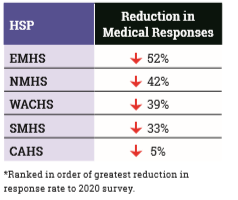
The 2020 survey saw a reduction in responses across all job roles, with the exception of Dental. However, medical practitioner responses reduced by a staggering 48 per cent.A total of 602 doctors completed the 2020 survey, compared to 1,159 doctors in 2019.
Many of the HSPs pointed to a focus on COVID-19 preparations as the reason for the reduction in the number of survey responses, which leads the Australian Medical Association (WA) to believe that WA Health should consider running the survey once again this year, to give medical practitioners the opportunity to share their opinions.
While COVID-19 may have served as a distraction, the great variation in the rates of reduction between HSPs and various job roles indicate that there may be other factors behind the drop in medical responses. The AMA (WA) points to medical practitioner disengagement as playing a role, in addition to the lack of perceived improvement following the 2019 results.
All medical practitioners should feel safe to speak up and challenge the way things are done in the organisation. Any alternative represents a risk to patient outcomes and health system efficiency.
The Child and Adolescent Health Service (CAHS) remains the front runner as having the highest proportion of doctors who feel safe to speak up and challenge the way things are done. Only the East Metropolitan Health Service (EMHS) has failed to improve the percentage of positive responses compared to the 2019 survey results. However, it continues to outperform the WA Country Health Service (WACHS), North Metropolitan Health Service (NMHS) and South Metropolitan Health Service (SMHS), all of which persistently underperform in a metric that is inherently connected to patient safety and financial efficiency.
NMHS and SMHS results indicate that 57 per cent and 61 per cent of doctors respectively, do not feel safe to speak up – results which warrant immediate, remedial intervention.
The AMA (WA) continues to point to the abuse of fixed-term employment contracts and the HSPs’ wilful failure to comply with public sector standards of probity and equity, particularly when appointing senior doctors, as contributing to the pervasive culture of fear which prevents doctors from speaking up.
Addressing these dire results is simple, cost effective and exists as a precedent for every other WA public sector employee – permanent employment.
Shared attitudes, values and beliefs
In 2019, the AMA (WA) reported on a number of questions that reflected the Association’s definition of culture – the shared attitudes, values and beliefs manifest in organisational behaviour.
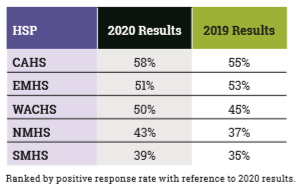
All the results reflect a similar pattern – improvements across all HSPs, with the exception of EMHS, noting that EMHS was, and continues to, outperform other HSPs in terms of positive responses (with the exception of CAHS).
While improvements have been made, the results at many of the HSPs continue to indicate a disengaged clinical workforce, with significant work required to produce clinical engagement levels that medical practitioners expect and deserve.
Comparisons between the HSPs show NMHS and SMHS continuing to underperform, while CAHS stands as an example to all other HSPs. The improvement in CAHS’ 2020 results marks a continuation of the remarkable transformation the health service has undertaken following the formal Health Department inquiry into the morale and engagement of PMH clinical staff. A success story WA Health should be proud of and other HSPs can learn from.