

Blog

It’s personal, all right!
Wednesday May 27, 2020
Healthcare workers (HCWs), including doctors, run toward COVID-19. After all, medicine is our calling, our identity and the profession that sustains our families and builds their future.
During this time, we face an unprecedented risk of becoming a statistic, or of making our loved ones sick. Around 0.7 per cent of infected persons (increasing with age) can be expected to die from this disease.1
There are more than 280 known infected HCWs in Australia who acquired the disease in the workplace.
We are all familiar with tragic reports of HCW deaths internationally, and in some cases inadequate PPE use contributed.2 At least 100 doctors are reported to have died from COVID-19 in Italy.3 This is an irreplaceable loss for 100 families, but also represents a team of medical care that is lost from the system forever.
We should do everything reasonable to prevent a replication of that disaster in Australia by targeting zero HCW infections at work. In Tasmania, the magnitude of the outbreak in Burnie was unforeseen.4 We do not have that excuse anywhere else in the country now that the epidemiological investigation report on the incident has been released.
PERSONAL PROTECTIVE EQUIPMENT (PPE): WHAT’S THE BIG DEAL?
Discussion around PPE has become emblematic of concerns of healthcare workers in relation to management response to COVID-19. In reality, PPE use is simply a lower-level frontline control, in a hierarchy of controls to manage the risk.
The reason PPE is thrown into sharp relief is that it is visible, and is to some degree in the hands, literally, of the individual HCW. This degree of control is not available to frontline staff in regard to higher-level, more effective methods of disease control.
PPE is like the bulletproof vest – a last line of defence, but much less useful than banning guns or metal detectors.
However, PPE like all personal equipment, has as large a role in providing psychological safety. It is a tangible indication that the organisation is protecting the individual and in the context of COVID-19, protecting their family and the wider health system. When the patient is positive and contact is unavoidable, PPE is the only control left to protect doctors and nurses from a highly infectious disease.
Our issues with the PPE policy stem from the guidelines themselves, the implementation and the result.
PPE GUIDELINES: AS MANY QUESTIONS AS ANSWERS
The Infection Control Expert Group (ICEG), advises the Communicable Disease Network of Australia (CDNA) and the Australian Health Protection Principal Committee (AHPPC)6,7,8, on guidelines for PPE. These authorities prefer that all other recommendations from the various colleges, associations and institutions submit to this advice.
The preamble to the CDNA guidelines states the evidence is poor, including in relation to workplace transmission in Australia. No responsibility is taken, nor attributable to, the experts making the recommendations. Frontline workers have had little to no say in the development of the guidelines, or their implementation – there has been no consultation with professional representative bodies like the AMA. Yet the burden of failure of the PPE is borne by the frontline worker.
There have been frequent changes to the guidelines since the onset of COVID-19. All of the iterations have reduced the requirement for more aggressive protective measures, with the result that less resource is required. This has led to distrust from HCWs, who do not see the evidence to support a shift away from aggressive protective measures as being any more convincing than it was at the outset. Many would prefer a more precautionary approach to this new and evolving disease risk.
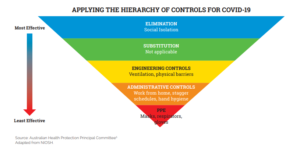
Examples of reduced PPE protection in these guidelines include:
- N95 masks no longer being required for aerosol-generating procedures unless in suspected or confirmed COVID-19 positive patients. This is in the setting of no pre-procedure testing of patients.
- The removal of any requirement for fit testing of N95 masks, which is mandated in the Australian Standard but not required in the guidelines, seemingly due to the administrative and resource burden that could result.
- Insistence that droplet precaution is not required for standard consultations.
- “Previous advice to use airborne precautions for the care of patients with severe coughing has been withdrawn because: o viral load does not necessarily correlate with the clinical condition
- coughing generates droplet predominantly, and
- surgical masks used by the patient, if possible, and healthcare worker provide adequate protection.”
The first two points here are expressed vaguely enough as to be pointless for application to many clinical scenarios.
The CDNA guidelines are based on the generally accepted view that most spread is by droplet or contact rather than by aerosol. This is where the 1.5m recommendation originates – when someone talks, then we are far enough to not get their droplets from speech in our face. This is an arbitrary cut-off and lacks the nuance that individual HCWs should be able to apply to their workplace depending on the clinical situation. Applying the 1.5m rule in many clinical situations is unrealistic and impossible.
However, if the droplet theory is not always correct, in even a small number of cases, then PPE should be more conservative due to the catastrophic potential of the risk. The precautionary principle would dictate higher-grade protection until more time has passed and more is certain about a new disease.
The guidelines do refer to the “supply chain” and “supply considerations” as influential in their formulation. However, these are not areas of expertise for the authors of the guidelines. They have to accept what they are told in relation to supply, and are not in a position to push back and say that the supply must simply be fixed or the work must not be done.
Companies outside of healthcare in other industries are not able to utilise the short supply of safety equipment as a reason to request the industry regulator to amend safety guidelines. They are required to meet the independent standard or cease operations. Accordingly, the incentive to meet the standard remains, and then with enough motivation, safety is maintained – as it could be with higher standard PPE in healthcare in Australia if enough resource was applied.
As a wealthy nation, we have the resources and the community goodwill to equip frontline workers with the world’s best PPE. In a time of low community spread, gained through a combination of aggressive lobbying, swift political decision-making and societal compliance, WA has the enviable opportunity to utilise very high standard PPE along with other controls to target zero healthcare worker infections.
Rather than aspire to this achievable outcome, the guidelines meekly state that things will be reviewed if the supply chain shifts. Anecdotal statements like “HCW infection in the workplace in Australia have generally occurred in situations where respiratory symptoms were present and PPE was not used” are made to bolster a lower standard than could and should be offered, although what is meant by “generally” is not detailed.
Powered Air Purifying Respirators (PAPR) are becoming widely available around the world and should be part of an aspirational standard. University Hospital Southampton in the UK has managed to provide locally-made devices to staff, and the response has been positive.
Australian manufacturers can do the same. The concerns from management about contamination on removal of the PAPR can easily be overcome with training as they are in every other jurisdiction.
Other factors that affect demand for PPE that are not mentioned in the guidelines, but which are nevertheless every bit as relevant as “supply chain” considerations, include:
- Whether the higher controls in the hierarchy are working –
- there is no current roadmap that sets out for example what degree of community spread would allow an upgrade of PPE; and
- there is no mention as to what will happen if PPE supply is running low at a local level, and whether higher protection would then be released.
- Workforce maintenance, the avoidance of quarantine, illness and resignations;
- Anxiety and mental health welfare concerns;
- Heterogeneity of patient interaction and sudden changes in clinical situations;
- Individual variation in vulnerability between healthcare workers who may have preexisting medical conditions;
- Fatigue and violation of safe working hours due to shortages and poor rostering;
- Different facilities, e.g. in General Practice and regional areas;
- Whether the system is overwhelmed with patient demand above census capacity for the facility. It is also not explicitly stated that these factors should be considered in the implementation of the PPE guidelines, and largely, they are not.
GUIDELINE IMPLEMENTATION: BUMPS IN THE ROAD
System managers tend to defer to “the guidelines” without qualification and simply mandate them as a maximum use of resources, rather than a minimum protection standard that can be increased as required to satisfy clinical and psychological concerns.
The fundamental problem with this approach is that the guidelines alone are a secondary aspect of the workplace health and safety framework. While they could act as an important tool, they do not supersede the Commonwealth and State Workplace Health and Safety legislation and regulations9 or employer obligations.
In particular, there is no change in the requirement on employers to exercise active management of risk, to discharge their duty of care to workers and patients. In WA, employers, health service provider boards and chief executives bear the legal liability of ensuring compliance with OSH standards, irrespective of what is contained in the guidelines.
Change management, consultation, open discussion and fair and equitable issue resolution are all legislated obligations. In the event that doctors challenge testing and/ or PPE protocols, management cannot discharge their obligations by simply referring to “the guidelines”.
The National Standards and manufacturer information for PPE are not altered or reduced by the presence of guidelines and where there is conflict, for example in the requirement for fit testing of respirators, the former prevail.
The system managers assume the rest of the system is working as designed, and that there is no overload of patients. Complaints from frontline workers about lack of protection have been dismissed as “chatter” by those in senior positions, and the preCOVID-19 cultural disconnect between workers and management in many of our health institutions has been exacerbated.
The well-documented high rates of burnout and disengagement result largely from a clash of command and control culture with the need for empathy, collaboration and communication that modern professionals rightly expect and on which patient outcomes depend.
There is a narrative of sacrifice in relation to healthcare, where the culture expects and relies on the workers to ‘step up’ and ‘do the right thing for the patient’ rather than complain about conditions, such as lack of access to the PPE that the HCW feels or knows they need.
While governments are prone to thanking workers publicly, quick to identify with the positive brand, they fail to listen to, let alone fulfil requests for better conditions. Yet they will attribute blame to workers when things go badly.
Training, and auditing the sufficient use of PPE is as important as procurement and preservation. The Tasmanian report included the important observation that critical priorities should include “our training, auditing and checking mechanisms to ensure that PPE is being worn appropriately at the right time and in the right situation in accordance with national guidance and local specialist infection control advice.”10
Doctors should make the reasonable request and advocate that they have available – at their discretion – best practice PPE (which is aspirational) in addition to the current guidelines, as follows:
- Droplet precautions for all patient interactions (surgical mask, gown, gloves, eye protection);
- In addition, fit tested and checked N95 respirator masks for all reasonably suspected or known COVID-19 patient interactions;
- Powered Air Purifying Respirators for aerosolgenerating procedures, and for all COVID ICU HCW.
Low-cost, high-volume production of N95 masks and PAPR devices should be incentivised immediately in Australia. Such aspirational standards would be rejected based on current guidelines, which rely on uncertain new science, and ignore important factors such as mental health, maintenance of the workforce, and the imperfect conditions and unpredictable nature of our own areas of frontline clinical care, in which each HCW is the expert. No one else.
Doctors should not waste PPE, but this can be accomplished through education and auditing rather than through administrative fiat. The current guidelines will predictably result in insufficient PPE in some circumstances because of the diverse and fluctuating clinical settings across all health services, and the changing processes across the state for procurement of PPE for the front line, including outside Health Department settings. Aged Care, private hospitals and General Practice have been left largely to fend for themselves.
THE RESULT: FRONTLINE DISTRESS & DIFFICULTY
Doctors know that they may be blamed unfairly for adverse outcomes and will be shamed or forced into working without adequate PPE. Wrongful assertions about workers possibly causing their own infections through flouting restrictions are reported as having been made by those in positions of authority, including the Chief Medical Officer of Australia.11
GPs in WA who did not want to see fever patients without PPE were also criticised by the State Health Minister who reportedly opined they were evading their moral and legal obligations.12 In fact, the GPs were properly analysing the risk to their practice, staff and other patients and acting on the duty of care to invoke a high level of control.
Some HCWs may try to use their own privately sourced PPE, but many have been told that this is not acceptable, even where the PPE meets and exceeds the guidelines and is TGA approved.
That reaction by a manager is probably not lawful or reasonable and the effectiveness and suitability should be analysed rather than the PPE rejected summarily. The purported problems with such an approach are not validated, and certainly not worse than HCW infection. If a health service cannot or will not provide PPE, it should either accept a reasonable substitute from the worker or provide other higher-level controls that remove the risk of COVID-19. The fact that HCW infections have already occurred at such high rates in Australia despite low overall incidence means the hierarchy of controls has failed.
Being forced to continue in unsafe work by one’s own moral code, or peer group pressure, because of a desire to continue caring for patients despite a lack of PPE, should be prevented through proper management.
Apart from infection, the mental health risks of post-traumatic stress disorder, moral trauma and anxiety are unreasonable. The provision of patient care should not come at the expense of HCWs’ physical and mental wellbeing, especially when such circumstances are entirely avoidable.
Subsequent legal claims for compensation may create further stress and complication not just for the HCW, but also individual managers who have their non-delegable duty of care in many instances under workplace health and safety laws.
The consequence of PPE insufficiency as a result of these issues could be more infection of HCW workers in the workplace, in addition to the 280 or so that have occurred during a relatively small case load in Australia so far. Some have already chosen to leave the workforce rather than risk it, and many more may follow if the full hierarchy of controls is insufficient, based on their personal evaluation. This could create major problems for the health system, well beyond shortages of PPE.
Already there is a dearth of cover for normal exigencies such as leave. Quarantine, illness and retirement add further pressure on remaining HCWs, leading to the system eventually spiralling into incapacity.
Now is the time for empathy, meaningful consultation and collaboration, aspirational as well as minimum standards, and a shift of power toward those who will use PPE as their last line of defence.
In WA, the involvement of Dr Chris Blyth and his working group – the COVID-19 Pandemic Infection Prevention and Control Advisory Committee – in these discussions is very encouraging. The AMA (WA) looks forward to working with the Committee and frontline doctors from all sectors to move the dialogue forward productively.
We will not settle for less than the best hierarchy of controls possible in this precious period of low case numbers, in order to target zero HCW infections being acquired at work. We will need to apply political pressure to attract the resource that our HCWs deserve, and certainly the AMA (WA) is up to that task – and we know the West Australian community is on our side.
References available upon request.

